eISSN 2444-7986
DOI: https://doi.org/10.14201/orl.18991
CASE REPORT
DEEP NECK INFECTION OF DENTAL ORIGIN. A CASE REPORT
Infección cervical profunda de origen dental. Descripción de un caso
Beatriz PARDAL-PELÁEZ
Doctor in Surgery and Dentistry. University of Salamanca. Department of Surgery. Salamanca. Spain.
https://orcid.org/0000-0001-5608-7924
Reception date: August 20, 2018
Date of Acceptance: August 29, 2018
Publication date: August 31, 2018
Date of publication June 1, 2020
Conflict of interest: The authors declare no conflicts of interest
Images: The authors declare that the images have been obtained with the permission of the patients
Rights policy and self-archive: the self-archive of the post-print version (SHERPA / RoMEO) is allowed
License CC BY-NC-ND. Creative Commons Attribution-Noncommercial-NoDerivate Works 4.0 International
University of Salamanca. Its commercialization is subject to the permission of the publisher
SUMMARY: Introduction and objective: At least 36% of deep cervical infections may have a dental origin. Case description: A 44-year-old woman who consulted for dysphonia of a week of evolution. Rhinofibrolaryngoscopy revealed left arytenoid edema and paralysis of the left hemilarynx and normal neck. A computerized axial tomography was performed, finding left parapharyngeal abscess. Systemic and surgical antibiotic treatment was performed with cervicotomy and drainage of the abscess in whose culture Prevotella buccae was isolated. Comments: The result of the culture helped establish the dental origin of the infection. In the dental history, a history of pericoronitis associated with 3.8 was found. Conclusions: The diagnosis of the dental origin of a deep cervical infection is established by dental history, oral examination, oral radiology and microbiological culture.
KEYWORDS: Deep Neck Spaces; Dental; Odontogenic; Abscess; Prevotella; Oral Microbioma; CARE; Equator Network.
RESUMEN: Introducción y objetivo: Al menos el 36% de las infecciones cervicales profundas pueden tener un origen dental. Descripción del caso: Mujer de 44 años que consultó por disfonía de una semana de evolución. La rinofibrolaringoscopia reveló edema aritenoideo izquierdo y parálisis de la hemilaringe izquierda y cuello normal. Se realizó una tomografía axial computarizada, encontrando absceso parafaríngeo izquierdo. Se realizó tratamiento antibiótico sistémico y quirúrgico con cervicotomía y drenaje del absceso en cuyo cultivo se aisló Prevotella buccae. Comentarios: El resultado del cultivo ayudó a establecer el origen dental de la infección. En la historia dental, se encontró una historia de pericoronitis asociada con 3.8. Conclusiones: el diagnóstico del origen dental de una infección cervical profunda se establece mediante la historia dental, el examen oral, la radiología oral y el cultivo microbiológico.
PALABRAS CLAVE: espacios profundos del cuello; dental; odontogénico; absceso; prevotella; microbioma oral; CARE; Equator Network.
Deep neck infections (DNI) usually originate in pharyngeal or oral infections. It is estimated that up to 36% of cases are of dental origin [1] as a result of periodontal disease [2] periapical abscesses without or with previous dental interventions [3] or radicular cysts [4].
The microbiota of infected root canals associated with acute apical abscess is polymicrobial, composed predominantly of Gram negative anaerobes (Phylum Firmicutes and Bacteroidetes [3].
Bacteria isolated in DNI can be classified into three groups according to their relationship with the oral microbiome [1,5]:
– Group 1: bacteria that are found in the oral microbiome and are responsible for oral pathology (caries, periodontal disease and oral infectious processes).
– Group 2: bacteria that are found in the oral microbiome but are not directly responsible for oral pathology.
– Group 3: bacteria not identified in the oral microbiome and whose culture therefore does not determine the oral origin of the DNI.
The diagnosis of DNI of dental origin is based on oral and radiological exploration and microbiological culture [1].
Objective
We present a case of DNI originated in the lower left third molar in which Prevotella buccae was isolated.
For the preparation of the case report, the CARE checklist was followed [6].
A 44-year-old Caucasian woman, with no previous medical conditions or treatments, who attended an otorhinolaryngology consultation for dysphonia with a progressive worsening of one week of evolution, without other local or general associated symptoms.
Rhinofibrolaryngoscopy showed left arytenoid edema and arytenoepiglottic fold and left hemilarynx paralysis. Normal neck. Oral treatment schedule was started with cefuroxime (500 mg / 12 h) and deflazacort (45 mg / 24 h).
Chest X-ray, cervicomediastinum computed tomography (CT) and blood analytical. The CT image showed the extension of the DNI from the left parapharyngeal space to the hypopharynx, preepiglottic space, left paraglottic space and retropharyngeal space (Figure 1).
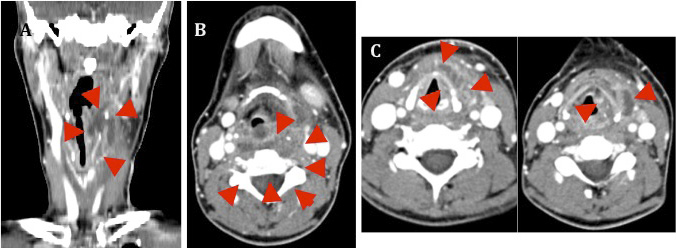
Figure 1. Deep cervical abscess of dental origin.
Coronal CT image (A). A. Image of the abscess that extends from the left peritonsillar and parapharyngeal space to the hypopharynx, the thyrohyoid (preepiglottic) space and the left paraglottic space.
Axial CT image at the level of hyoid bone (B) and larynx (C). B. The extension of the abscess towards the left parapharyngeal, retropharyngeal and preepiglottic spaces indicated with arrows is observed. C. Abscess that affects the prethyroid area and the left paraglottic space.
Until the completion of the CT scan, the symptoms were progressive, requiring urgent hospital admission for dyspnea.
Left cervicotomy and drainage of the abscess were performed under general anesthesia with orotracheal intubation. Samples were taken for aerobic and anaerobic bacteria culture.
The intravenous antibiotic treatment prescribed from the emergency area was with amoxicillin / clavulanic acid 1000/200 mg (at a dose of 2 g every 8 hours). That was maintained up to ten days after the postoperative period.
The patient remained in the intensive care unit (ICU) for 3 days being extubated at 24 hours.
In the anaerobic culture, Prevotella buccae was isolated, so the patient’s dental history was reviewed, which showed processes of chronic pericoronitis associated with 3.8, which could be identified in a panoramic radiograph obtained six years earlier (Figure 2). The aerobic culture was negative. Prevotella buccae was resistant to penicillin G and sensitive to amoxicillin / clavulanic acid, piperacillin / tazobactam, imipenem, clindamycin, chloramphenicol and metronidazole.
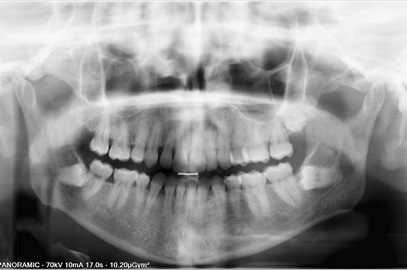
Figure 2. Panoramic radiography obtained after deep neck infection. No radiographic changes are detected in left lower third molar.
A new panoramic radiograph was performed which did not provide relevant information regarding the previous one. One month after discharge, the extraction of 3.8 was performed.
The evolution was favorable with absence of postoperative infection and recurrence of DNI after 47 months of follow-up.
Prevotella buccae is the strict anaerobic bacterium Gram negative [4] most prevalent in periodontal disease [2], it is usually present in the microflora of the mouth, the gastrointestinal tract and the vagina [7]. It is also found in oral bacterial plaque [8], in periodontal pockets in 60.4% of cases [2], in radicular cysts [4], in periapical abscesses in non-endodontically and necrotic teeth [3] and in odontogenic abscesses [3,4,9].
Infections originate in the periapical area of the tooth and the absence of dental treatment can lead to polymicrobial cervical infections [4].
Other species have been isolated in dental and periodontal infectious diseases, such as P. denticola, P. intermedia or P. melaninogenica (39.6%, 35.4% and 22.9% respectively) [2]. Prevotella ssp is isolated in 3.6% of cultures in ICP [1]. The relative risk of finding P. buccae in an odontogenic abscess is 2.86 and in an infiltrate 2.94 [9].
The proteolytic activity of P. buccae (and especially of P. intermedia and P. nigrescens) explains its ability to extend through the cervical planes [4]. Prevotella spp, F. nucleatum and S. anginosus are involved in the pathogenesis of odontogenic abscesses [9]. P. buccae, P. oris, P. intermedia and P. oralis predominate in large abscesses [9].
Prevotella spp has also been isolated in periapical abscesses in non-endodontized and necrotic teeth (P. buccae in 50%, P. nigrescens in 40%, P. tannerae in 20% and other genera in 15%) [3].
In the case presented, the isolation of P. buccae was determinant to establish the dental origin of the infection, as it belongs to group 1 [1].
However, most of the DNI are polymicrobial and the isolated bacteria belong to group 2 and the dental cause can be underestimated, which is why intraoral exploration by a dentist and the review of dental history are necessary to rule out chronic oral pathological processes in patients with DNI [1].
The case presented is an example of DNI with severe progressive symptoms that began with dysphonia and left laryngeal paralysis in which the dental origin was established after the isolation of Prevotella buccae in the culture of the sample obtained from the abscess by cervicotomy and drainage.
It is necessary to systematize the criteria for the diagnosis of DNI including oral examination, dental history, oral radiology and microbiological culture to establish their possible dental origin.
A greater preventive activity on oral pathologies (caries, periodontal disease and oral infectious processes) could reduce the incidence of DNI of dental origin.
This article is published with the express permission of the patient.
The author make public the gratitude to the professionals involved in the diagnosis and treatment of the patient: the ICU staff, the Otorhinolaryngology Service and the Microbiology Service of the Zamora Healthcare Complex (Spain), the “Q-Diagnostica” Radiodiagnosis Unit from Zamora (Spain) and Dr. M. Ruth Olmo Velasco and Dr. Mercedes Rojo from Zamora (Spain) for providing access to the patient’s dental history and the Recaver dental clinic in Valladolid (Spain) for the completion of dental treatment.
1. Pardal-Peláez B, Pardal-Refoyo JL, Ochoa-Sangrador C, González-Serrano J, Montero-Martín J, López-Quiles J. Analysis of the prevalence of dental origin of deep neck infections. J Oral Maxillofac Surgery, Med Pathol. 2018 Mar;30(2):180–6.
2. Maestre JR, Bascones A, Sánchez P, Matesanz P, Aguilar L, Giménez MJ, et al. Odontogenic bacteria in periodontal disease and resistance patterns to common antibiotics used as treatment and prophylaxis in odontology in Spain. Rev Esp Quimioter [Internet]. 2007 Mar;20(1). Available from: http://www.seq.es/seq/0214-3429/20/1/61.pdf
3. Nóbrega LMM, Montagner F, Ribeiro AC, Mayer MAP, Gomes BPFA. Molecular Identification of Cultivable Bacteria From Infected Root Canals Associated With Acute Apical Abscess. Braz Dent J. 2016 Jun;27(3):318–24.
4. Tek M, Metin M, Sener I, Bereket C, Tokac M, Kazancioglu HO, et al. The predominant bacteria isolated from radicular cysts. Head Face Med [Internet]. 2013 Sep;9(1):25. Available from: http://head-face-med.biomedcentral.com/articles/10.1186/1746-160X-9-25
5. Chen T, Dewhirst FE, Paster BJ, Tanner A, Wade W. HOMD: Human Oral Microbiome Database [Internet]. All Human Oral Microbial Taxa. 2017 [cited 2017 Nov 25]. Available from: http://www.homd.org/
6. Gagnier JJ, Kienle G, Altman DG, Moher D, Sox H, Riley D, et al. The CARE guidelines: consensus-based clinical case reporting guideline development. BMJ Case Rep [Internet]. 2013 Oct 23 [cited 2017 Nov 4];2013. Available from: http://www.ncbi.nlm.nih.gov/pubmed/24155002
7. Yanagisawa M, Kuriyama T, Williams DW, Nakagawa K, Karasawa T. Proteinase activity of prevotella species associated with oral purulent infection. Curr Microbiol. 2006 May;52(5):375–8.
8. McBain AJ, Bartolo RG, Catrenich CE, Charbonneau D, Ledder RG, Gilbert P. Growth and molecular characterization of dental plaque microcosms. J Appl Microbiol. 2003;94(4):655–64.
9. Cachovan G, Blessmann M, Schön G, Rother U, Heiland M, Stürenburg E, et al. Radiography-based score indicative for the pathogenicity of bacteria in odontogenic infections. Acta Odontol Scand. 2014 Oct;72(7):530–6.